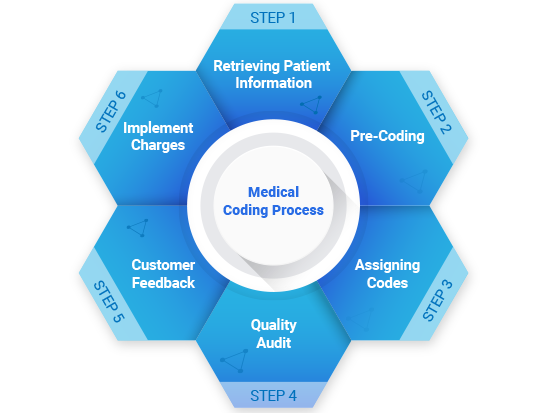
At Baruch Business Solutions (BBS), we understand the intricate and technical process of Medical Coding through and through. As the norms and legislative guidelines are constantly changing – Medical Coding is one of the most complex and important aspects of medical facilities like hospitals, clinics, individual physicians, surgeons, and diagnostic laboratories. We at BBS ensure pin-point accuracy of the medical code which materializes after a meticulous analysis of the patient’s medical data. Our coding specialists perform their tasks with the highest accountability possible and push your business revenue up the financial graph. With time it is becoming clear that Medical Coding is a responsibility which should be handled by experts who are well-versed with thousands of medical codes present in the current scenario – with constant amendments and updates. Keeping track of all these changes is a huge administrative burden and therefore needs to be dealt with by professionals. Not only does a specialized medical coder assure increased profits by thousands of dollars but also keeps at bay the legal implications arising out of incorrect coding.
Our coders and auditors are the American Academy of Professional Coders (AAPC) certified and have several years of experience. Keeping up with the latest code guidelines and norms – our auditors remain alert and well-educated about the ever-reforming coding trends. Our team makes sure that constant denials become history and a seamless revenue flow is achieved; making the profits surge. Our coders and auditors follow every standard possible like LMRP, ICD-10- CM, HCPCS Level II, and CPT Assistant to name a few.
At BBS precision matters, we have integrated technology-based systems in our processes to analyze the medical data that is provided to us. A comprehensive study of the medical documentation is done by competent coders so that financial setbacks due to denials, reimbursement issues, late payments, rejections, and inaccuracies are seized. Using electronic means, our team of experts can foresee any discrepancies in the documentation, thereby curbing revenue losses due to errors in Medical Coding. The efficient use of software, technology, and standardization of processes helps in keeping the complicated process of Medical Coding transparent, secure, and having high data-integrity. Be it your clinic or a large hospital, hiring a Medical Coding expert takes a tremendous burden off your shoulders and leaves you with a relaxed state of mind. While we handle the hassles of coding, you can completely focus on your medical care business. Our team lays special focus on Revenue Cycle Management (RCM) of your medical facility by performing thorough research to fix every shortcoming.
Our professional medical coders are highly skilled and strive to stick with the official HIPAA-mandated code sets serving different needs. The standards we cover are as follows,
- ICD-10-CM (International Classification of Diseases, 10th Edition, Clinically Modified)
- CPT ® (Current Procedural Terminology)
- ICD-10-PCS (International Classification of Diseases, 10th Edition, Procedural Coding System)
- HCPCS Level II (Health Care Procedural Coding System, Level II)
- CDT® (Code on Dental Procedures and Nomenclature)
- MS-DRG (Medical Severity Diagnosis Related Groups)
- APC (Ambulatory Payment Categories)
- NDC (National Drug Codes)
The edge you get with BBS:
- Highly competent auditors and coders that specialize in every Medical Coding norm, standard, and legislative guideline.
- Customized and tailored Medical Coding solutions that suit your medical-care business needs.
- Proficient use of technology and automation to maintain a high percentage of accuracy, tracking, and data integrity.
- Revenue Cycle Management (RCM) based analysis focusing on the cause of revenue losses and its solution.
- Removing denials, reimbursement/payment delays, and legal issues by foreseeing documentation errors and their impact.